Portions of this article are excerpted and adapted from the upcoming bookHope Against Hope, authored by Renascent’s Clinical Director Michael Lochran and consulting Psychotherapist Laura Cavanagh. Hope Against Hope is scheduled for publication later this year.
Adolescence and early adulthood are developmental periods of particularly high risk for the development of substance use and addictive disorder (see Part One for more). Many concerned family members contact us, unsure of whether the young person in their life is experimenting with substances like many of their age, or whether they are on their way to developing a serious addictive disorder.
Often there is a hope that as the young person gets older, they will begin to moderate their use. And some people do gradually decrease the frequency and intensity of their drug or alcohol consumption in early or middle adulthood. But addiction becomes more treatment-resistant the longer that it progresses, and it is often the case that the window in which intervention would have been especially effective is missed as family members and loved ones wait in the hope that the young person will simply outgrow their addiction.
So what signs are there that a young person is not simply experimenting, but actually at risk of developing a serious substance-use disorder? And what are the signs that it’s time to seek help?
The Gateway Drug Model
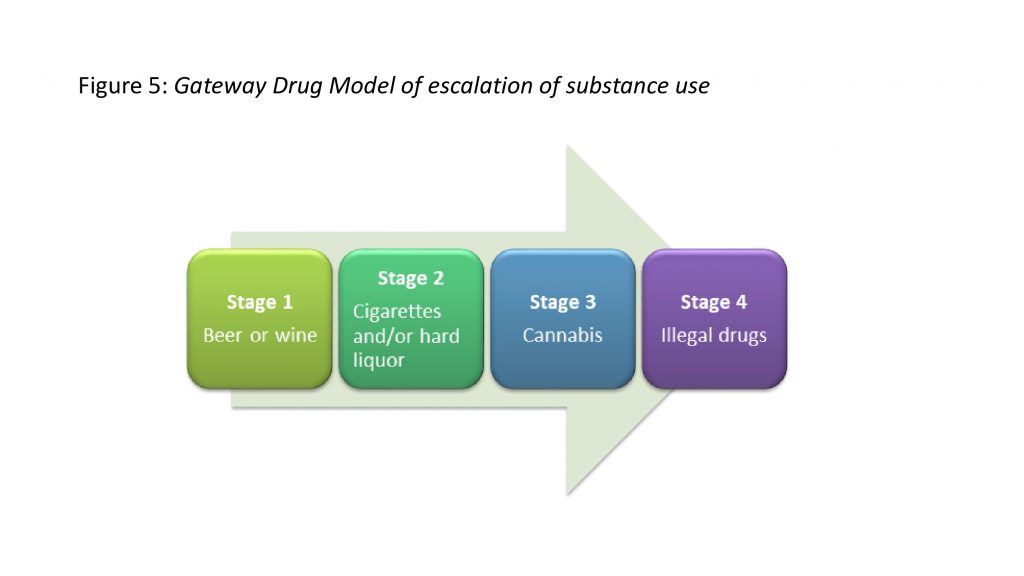
The Gateway Drug Model is a model that focuses on the types of drugs used, and that when someone crosses a line to using illegal drugs, then it is time to seek help. In 1975, Dr. Denise Kandel of Columbia University proposed a sequence of drug use initiation that involved at least four stages from non-use to hard drug use (Kandel, 1975; Kandel & Faust, 1975).
These stages, marked by type of drug, were as follows:
1. Beer or wine
2. Cigarettes or hard liquor
3. Marijuana
4. Oher illicit drugs
(Source: Kandel & Faust, 1975, p. 923; see Figure 1).
Kandel observed that almost no teens tried marijuana who had not experimented with alcohol or alcohol and tobacco. She noted that 26% of adolescents who progressed to using marijuana would move on to stage 4, but that only 1% of teens who did not use marijuana would try illicit drugs. She believed that progression from one stage to the next could be predicted by intensity and frequency of use at the previous stage. She further hypothesized that at each stage tolerance and reduced sensitivity leads the teen to seek out stronger and stronger substances.
Although many people may have followed a similar sequence in the beginning stages of experimentation with substance use, the Gateway Drug Model has been widely criticized in terms of both its validity and utility in predicting who is at risk of starting hard drug use. For example, a 15-year-old who has been binge drinking since age 13, but who has never tried marijuana may be at higher risk of saying yes to a club drug, compared with a 15-year-old who has tried both alcohol and cannabis, but only recently and only in moderation.
The predictive validity of the Drug Gateway Model breaks down when the typical use of drugs are taken into account. Approximately 75% of Canadian teenagers have tried alcohol. If 75% of the population meets the first two stages, it is hard to argue that this is indicative of a developmental progression towards stage 3, even if most of those who reach stage 3 have gone through stages 1 and 2. If nearly everyone goes through stages 1 and 2, the fact that someone who is in stage 3 has gone through stages 1 and 2 may be more coincidental. Although almost all teens who try marijuana have tried alcohol and cigarettes, this is not particularly helpful information when almost all teens have tried alcohol or cigarettes. Far better predictors of risk exist, including number of adverse childhood experiences and age (rather than substance) of first use.
What about the progression from marijuana to hard drugs? When the frequency of marijuana use within the population is factored in, the strength of the predictive model decreases. For example, in Japan, cannabis use rates are very low. One cross-cultural study found that 83% of hard drug users in Japan had not used cannabis first (Degenhardt et al., 2010).
Passing through the tobacco “gateway” may be less common for youth today than it was two decades ago. While teen smoking rates have decreased dramatically over the last two decades, rates of cannabis use have increased. Canadian youth use more cannabis than teens in any other country in the world – eleven times more (Government of Canada, 2019; Patel & Marwaha, 2020). Policies influenced by the Drug Gateway Model were predicated on the notion that decreasing use of the gateway drugs would lower the risk of teens moving to more advanced stages. Clearly, a decrease in teen smoking did not lead to a decrease in teen marijuana use. Recent trends in cannabis use indicate that access, availability, and social norms are better predictors of use than the Drug Gateway Model.
The Gateway Behaviour Model
With the Gateway Drug Model having limited clinical utility, we need to look to other models to predict the pathways to addiction. A behavioural model is more practical in that it looks at the individual holistically, rather than just their behaviour around a particular drug. The use of street drugs does not necessarily predict addiction. An adolescent may never try illegal drugs, but may still develop a disabling cannabis- or alcohol-use disorder. Another may try ecstasy, ketamine, and psilocybin along with alcohol and cannabis, and not develop an addiction to any of these.
So what would be the key behavioural markers that could be used as milestones in a gateway behaviour model of addiction? What are some signs that would indicate that a young person is progressing towards a serious substance-use disorder? What indicators would let us know that early intervention is necessary?
- 1.Early Warning Indicators
In the earliest stage, age of first use represents a reliable predictor of increased risk for substance-use disorders. This is an objective, observable marker that should be taken seriously in terms of early intervention and preventative support strategies. There seems to be a protective effect with each year of delayed first use for those under the age of 18, with the youngest first-time users having higher risk of addiction even compared to those whose first-time use occurred at just one year older (Chen, Storr & Anthony, 2009).
Prior to first use, risk factors include number of adverse childhood experiences and family history of addiction. Whether or not the child seems “affected” is irrelevant; these are predictive factors in identifying those most vulnerable in the future, whether or not the child appears to be coping well in the present.
2.Enhanced Drug-Seeking
What objective behaviours might indicate that someone is at high risk? These are called behavioural determinants and may include poly-substance use. Using more than one drug, regardless of the drugs used, would be an objective measure of enhanced drug seeking. Poly-drug use represents greater liability for addiction, and indicates an overall enhanced desire to seek out altered states. Even within opioid addiction, the number of different opioids used represents a risk factor for progression to heroin use and intravenous drug injection (Grau et al., 2007). Number of substances used (rather than types of substances used) would be the indicator of risk, with a higher number indicating greater risk.
In adolescence, purchasing of substances (as opposed to taking what is on offer) would be an indicator of enhanced drug-seeking. Similarly, so is getting drugs for future use. There is a difference between those who are getting something for a particular occasion (buying alcohol to bring to a party) from those who are building a stockpiled supply (buying alcohol to hide in my room in case I feel like drinking). This teen hiding alcohol or other drugs is quickly transitioning to regular use. They are also beginning to show the impulsivity characterized by addiction: that the thought of wanting to use and having to wait is unbearable.
In his excellent book Beautiful Boy (now a major motion picture), David Sheff (2008) recounts his son Nic’s battle with the disease of addiction. Nic is a poly-drug user, although his drug of choice is meth. Sheff describes finding his son’s stash of marijuana when Nic is just 12 years old. Concerned, Sheff reaches out for advice from a teacher. The teacher tells him not to worry because Nic’s grades are good, and experimentation with drugs is normative for teens. A lack of understanding of the behavioural progression of drug use leads both Sheff and the teacher to ignore the serious red flags on display in this anecdote. Consequences like compromised academics tend to come much later in the progression of drug use, when addiction is far more resistant to treatment. By the time Nic actually fails out of school, he is already an intravenous meth user. Had Sheff and the teacher known more about behavioural gateway markers, they would have recognized a need for immediate intervention. That Nic is already using two substances (alcohol and cannabis), is purchasing his own substances, and is storing them for future use indicates that he is far off the path from normative use for his age. At 12, he reached Stage 2. In addition, he is already in a higher risk category due to his adverse childhood experiences (acrimonious parental divorce) and his young age of first use.
3.Non-Normative Drug Use
Drug use that veers off from normative adolescent use should also be considered a gateway behaviour. Using alone (as opposed to social use) is not normative for teens and indicates an elevated risk for the development of substance use disorder. Using at non-normative times or in non-normative situations would indicate elevated risk as well. This might include using in the morning or using before going to the gym. Using for the express purpose of intoxication is a behavioural marker that indicates cause for concern. Using for relief of stress, sadness, anger or anxiety, or using to manage other psychological symptoms would also be a cause for concern. This pattern of use comes before rapid behaviour escalation as substance use heightens the symptoms that the user is attempting to relieve (Ahmed et al., 2002; Childs, O’Connor, & DeWit, 2011; Koob, 2013). Failed attempts to adjust using patterns to match the normative use of one’s peers would be a sign of continued progression.
4.High-Risk Substance Use
In this stage, the individual has progressed towards addiction. These behavioural markers would indicate serious risk and signal a need for immediate intensive intervention. Daily use is a behavioural marker of serious concern. Daily use means substance use overall, not the use of any one particular drug. An individual who drinks alcohol on weekends and uses cannabis during the week is a daily user, even though they do not use the same substance every day. Using at school, work or in other settings where use is not sanctioned and could lead to consequences would also be high-risk behaviour. Illegal drug use indicates advanced progression, as does intravenous drug use (Hansen, 2013). For alcohol and benzodiazepine users, blackouts – where the user has periods when they are intoxicated that they cannot recall post-intoxication – is also a high-risk bio behavioural indicator of addiction (Miller et al., 2019).
5. Consequences from Substance Use
Negative consequences tend to occur further along in the progression than people might think, as illustrated in Sheff’s example above: parents and teacher assumed that if Nic’s use was high-risk his grades would be suffering. In fact, consequences tend to occur deep in the progression of the disease rather than leading up to it. Serious consequences are an indicator that the individual is either in or past the early stages of the disease of addiction. Early consequences would include poor performance at school or work or disciplinary action at school or work (e.g., from getting caught with drugs on one’s person). Delinquency in general indicates an elevated risk of addiction (Tarter et al., 2006). Impaired driving, violence (whether as victim or perpetrator), or injury when intoxicated would be other examples of high-risk consequences. Overdose (sometimes referred to as alcohol poisoning in the case of alcohol) or psychosis (for stimulant or hallucinogen users) are other behavioural indicators of risk.

In contrast to the gateway drug model, this model uses behavioural markers to indicate increasing level of risk and progression along a developmental trajectory towards addiction.
A Gateway Behavior Model of addiction has greater uses in predicting risk and in understanding the path towards addiction that differs from normative patterns of use. Even in the earliest stage, we can identifyrisk. Although the majority of teens drink, the majority of 13 year-olds do not (Government of Canada, 2020). Understanding and recognizing signs of risk can help professionals, individuals, and their families to identify a need for intervention and help them find the support they need.
Renascent Can Help
If you are worried about yourself or a young person in your life, do not wait. Call us today. Our experienced intake counsellors can assess whether someone is at risk, and the extent of the progression of their disorder, from mild to severe. Based on the assessment, our intake team will work with you to determine which of our programs are best suited to meet your needs. We are experienced in working with clients of all ages, and are especially committed to helping young people face the unique struggles of coming into recovery at an early age. Contact us today to find out if we can help. Recovery is possible.
Selected References
Ahmed, S. H., & Koob, G. F. (2005). Transition to drug addiction: a negative reinforcement model based on an allostatic decrease in reward function. Psychopharmacology, 180(3), 473-490. 10.1007/s00213-005-2180-z
Cavanagh, L. & Lochran, M. (2022). Hope against hope: Addiction, treatment, and recovery. Toronto, ON: McGraw Hill.
Chen, C., Storr, C., & Anthony, J. (2008). Early-onset drug use and risk for drug dependence problems. Addictive Behaviors, 34(3), 319–322. https://doi.org/10.1016/j.addbeh.2008.10.021
Childs, E., O’Connor, S., & De WIt, H. (2011). Bidirectional interactions between acute psychosocial stress and acute intravenous alcohol in healthy men. Alcoholism Clinical and Experimental Research, 35(10), 1794-1803. https://doi.org/10.1111/j.1530-0277.2011.01522.x
Degenhardt, L., Dierker, L., Chiu, W., Medina-Mora, M. E., Neumark, Y., Sampson, N., Alonso, J., Angermeyer, M., Anthony, J. C., Bruffaerts, R., de Girolamo, G., de Graaf, R., Gureje, O., Karam, A. N., Kostyuchenko, S., Lee, S., Lépine, J., Levinson, D., Nakamura, Y., Posada-Villa, J., Stein, D., Wells, E., & Kessler, R. (2010). Evaluating the drug use “gateway” theory using cross-national data: Consistency and associations of the order of initiation of drug use among participants in the WHO World Mental Health Surveys. Drug and Alcohol Dependence, 108(1), 84–97. https://doi.org/10.1016/j.drugalcdep.2009.12.001
Government of Canada. (2019, December 13). Canadian Cannabis Survey 2019 – Summary. https://www.canada.ca/en/health-canada/services/publications/drugs-health-products/canadian-cannabis-survey-2019-summary.html#s2
Government of Canada. (2020, October 26). Table 12. Past twelve-month use and mean age at first use of alcohol and cannabis, by grouped grades, Canada, 2018-19. https://www.canada.ca/en/health-canada/services/canadian-student-tobacco-alcohol-drugs-survey/2018-2019-detailed-tables.html#t12
Grau, L., Dasgupta, N., Harvey, A., Irwin, K., Givens, A., Kinzly, M., & Heimer, R. (2007). Illicit use of opioids: Is OxyContin® a “gateway drug”? The American Journal on Addictions, 16(3), 166–173. https://doi.org/10.1080/10550490701375293
Hansen, W. (2014, May). Estimating the risk of gateway drug behaviors: Using attitudes to model risk of future use by adolescents [Conference paper]. Society for Prevention Research, 22nd Annual Meeting 2013, Washington, DC. https://www.researchgate.net/publication/268125392_Estimating_the_Risk_of_Gateway_Drug_Behaviors_Using_Attitudes_to_Model_Risk_of_Future_Use_By_Adolescents
Kandel, D. (1975). Stages in adolescent involvement in drug use. Science (American Association for the Advancement of Science),190(4217), 912–914. https://doi.org/10.1126/science.1188374
Kandel, D., & Faust, R. (1975). Sequence and stages in patterns of adolescent drug use. Archives of General Psychiatry, 32(7), 923–932. https://doi.org/10.1001/archpsyc.1975.01760250115013
Kandel, D., & Yamaguchi, K. (1993). From beer to crack: developmental patterns of drug involvement. American Journal of Public Health, 83(6), 851–855. https://doi.org/10.2105/ajph.83.6.851
Koob, G. F. (2013). Addiction is a reward deficit and stress surfeit disorder. Front Psychiatry, 4(72), 10.3389/fpsyt.2013.00072
Miller, M., DiBello, A., Meier, E., Leavens, E., Merrill, J., Carey, K., & Leffingwell, T. (2019). Alcohol-induced amnesia and personalized drinking feedback: Blackouts predict intervention response. Behavior Therapy, 50(1), 25–35. https://doi.org/10.1016/j.beth.2018.03.008
Patel, J., & Marwaha, R. (2020). Cannabis Use Disorder. InStatPearls. StatPearls Publishing.
Sheff, D. (2008). Beautiful boy: A father’s journey through his son’s addiction. Boston: Houghton Mifflin Harcourt.
Tarter, R. E., Vanyukov, M., Kirisci, L., Reynolds, M., & Clark, D. (2006). Predictors of marijuana use in adolescents before and after licit drug use: Examination of the gateway hypothesis. The American Journal of Psychiatry, 163(12), 2134–2140. https://doi.org/10.1176/ajp.2006.163.12.2134

